1. San Francisco Street Crisis Response Team Has Responded To Over 70,000 Calls For Service.
San Francisco, California’s Street Crisis Response team recently marked its fifth anniversary and hit a major milestone—having responded to more than 70,000 calls for service as of January, the city’s team tracker reported. The mobile crisis team was included in a Harvard report highlighting some of the most robust crisis response programs in the country. Here’s a look at the city’s data below (you can visit their monthly reports and dive deeper here):
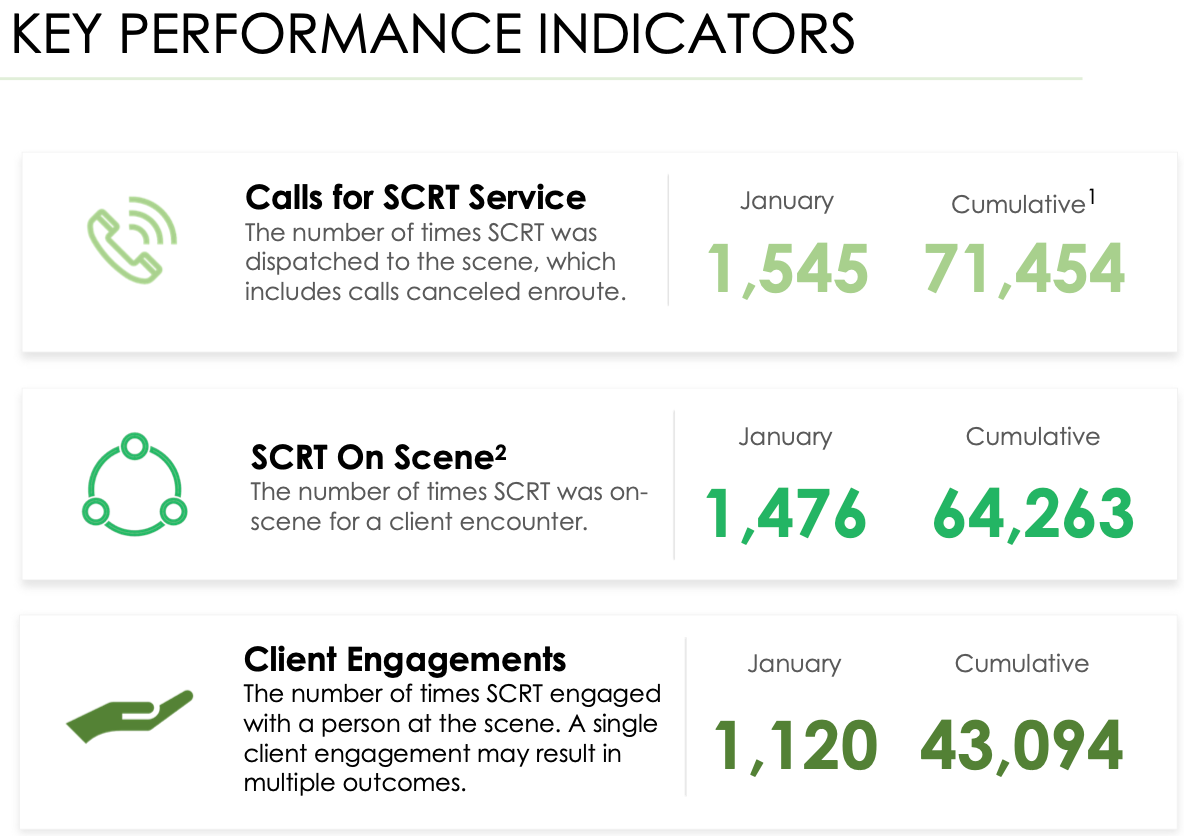
The Street Crisis Response Team, piloted in 2020 and expanded since, is now composed of “one community paramedic, an EMT or second paramedic, and either a Peer Counselor or a Homeless Outreach Team specialist” and is deployed “through calls from the public to San Francisco’s 911 call center… seven days a week, 24 hours a day.” The SCRT is part of an effort to provide appropriate medical and mental health care to residents “while reducing unnecessary law enforcement responses and unnecessary emergency room utilization.”
The team also provides “linkages to shelter, drug and alcohol sobering centers, mental health clinics and residential programs.” And in the days and weeks that follow a call for service, responders also provide “follow-up and connection to behavioral health care for clients.”
Researchers examining the program also found that the team “has accomplished some major [performance] milestones… a stable response time [] that compares favorably to police response… clients [who] are either connected to the appropriate medical and mental health services or [] through direct services and referrals for future interventions… [and] the portion of behavioral health crisis calls diverted through police dispatch has increased.” That’s why, researchers noted, “SCRT is already proving to be a leader in this collaborative and innovative work… consulting with other jurisdictions contemplating similar programs on both a national and international stage.”
Momentum For Mobile Crisis Response Teams Around The Country:
- The University of Washington Launches Campus Mobile Crisis Team, “Shifts Crisis Response Model Away From Law Enforcement.” For The Daily, Sophia Sostrin reports on the university’s “new approach to on-campus crisis response” called Husky Assist, “a mobile mental health crisis response team … [that now] sends trained clinicians—rather than law enforcement—to certain behavioral health emergencies.” The team, composed of trained mental health experts “all with master’s degrees in mental health fields,” was created after researchers at the university examined crisis response call logs from the university-run hotline as well as University of Washington Police Department and found that “many calls did not warrant an armed police presence.” When someone on campus calls 911 or the university hotline for help, trained dispatchers “who are not police officers, assess each situation and decide whether to send [the mobile crisis response team], [or] law enforcement… based on structured questioning,” similar to the protocols that cities that have embedded mental health clinicians into the 911 emergency call center follow. UW joins a growing number of universities that are launching their own mobile crisis response teams including University of California, Berkeley; California State University, Long Beach; and Oregon State University.
- In St. Clair County, Michigan, Mobile Crisis Team Expanding With New Vans For Enhanced Call Response. For The Port Huron Times Herald, Andy Jeffrey reports on the new vans that “provide a private, controlled space for assessments, conversations and de-escalation.” Inside, the vehicle is outfitted with comfortable seating for mental health responders as well as patients… “and internet connectivity that allows clinicians to connect virtually with a physician or prescriber for medication reviews.” The van is also equipped with supplies like food, water, medical supplies and “a refrigerator for temperature-sensitive medications.” Leslie Brown, program supervisor for the mobile crisis unit, explained that “before the van… staff often had to meet people in unpredictable environments… [often without] a safe place to speak with people [already in crisis]… now, someone can come into the van, warm up and talk” and receive treatment without having to be taken to a facility.

- In Eureka, California, CARE Team Expands Coverage Across Unincorporated Areas Of The City. For Left Coast Outpost, Sage Alexander reports on the CARE team, which “responds to calls for mental health or substance use” and is deployed through 911 dispatch, is now taking over response for unincorporated areas of Eureka—an expansion that increases the population served by the team from 40 percent to 60 percent. The team, composed of mental health clinicians and case managers, launched in 2023 as a pilot but has since become part of the fabric of the city’s public safety infrastructure, now responding to calls 7 days a week, 8AM to 7PM, relieving strain on law enforcement.

2. Report: States Are Using Smarter Policy Tools To Grow The Behavioral Health Workforce.
As demand for behavioral health services continues to surge, communities across the country face a severe shortage of qualified providers—creating urgency around scalable ways to recruit, train, and retain workers quickly. A new analysis from The Pew Charitable Trusts notes that roughly 40% of Americans, about 137 million people, live in areas with shortages of mental health providers, with rural and low-income communities facing the deepest gaps. Pew says states are increasingly turning to targeted policy tools to close those shortages and strengthen crisis-care capacity. The full report is worth your time, but here are some toplines on how state leaders can help close these gaps:
- Build career pipelines earlier. States can create pipeline programs that help students and current workers “begin or advance their careers” through education funding, mentoring, and professional development. Pew says these initiatives have already “meaningfully addressed workforce shortages” in some states and increased the number of underrepresented providers.
- Loan repayment and scholarship programs can help providers choose shortage areas. Pew notes these incentives have already been effective in “recruiting and retaining providers,” while some programs offer clinicians up to $50,000 in educational loan repayments for serving high-need communities.
- Conduct “comprehensive data analyses to identify needs and priorities” and use it to understand the “supply and demand of the state’s behavioral health workforce,” so that state and local leaders deploy resources where shortages are most acute.
State And Local Leaders Already Expanding The Behavioral Health Workforce:
- Utah Launches Behavioral Health Workforce Accelerator Program. Tech Buzz News reports on the state’s new accelerator program “to expand the behavioral health workforce, offering funded licensure support, training, and career pathways to address clinician shortages” with programming tailored to the needs of the states of Illinois, Kansas, and Michigan. The program offers up to $8,500 per participant covering “exam prep, fees, peer support, job-site training, and structured career development” with the goal to “move more candidates through licensure and into high-need community settings faster,” tackling a major chokepoint where “more than half of master’s-level therapists never make it to licensure.”
- Los Angeles “Universities Get $110 Million To Shore Up Mental Health Workforce.” For LAist, Robert Garrova reports on a $110 million investment from the Ballmer Group to UCLA, Cal State University-Los Angeles and Cal State University-Dominguez Hills “to support the training of new mental health workers.” The funding “will go toward scholarships of up to $18,000 a year for students studying in fields related to mental health… [as well as] launch a new program that aims to train hundreds of mental health workers to focus on South L.A. neighborhoods.” The universities told the news station that the “investment will support hundreds of behavioral health graduates over the next five years.”
- Albuquerque Community Safety Department Expands Crisis Response Workforce Through Latest Responder Academy Cohort. Albuquerque Community Safety Department announced the launch of its second responder academy of 2026, bringing in new trainees for intensive instruction and field training. The city says recruits are being prepared to respond to “behavioral health crises, substance use concerns, homelessness, suicidal ideation and other non-violent emergencies” through training in “trauma-informed care, de-escalation strategies, crisis communication, and resource navigation.” After graduation, the new class will help meet “the growing demand for non-emergency calls routed through 911 and 311,” building on a department that has already handled more than 149,000 calls since launch.

3. Cities Opening New Crisis Stabilization Centers To Reduce Reliance On ERs, Jails.
- Utica, New York, Opens 24/7 Crisis Stabilization Center “To Relieve Burden On [] Emergency Rooms, Police” For WKTV, Kirk Tupaj reports that Utica has opened a new Supportive Crisis Stabilization Center that is “open 24/7 for anyone in crisis,” including mental health and substance-use emergencies. Officials say peer-based staff can help with “stress, anxiety, depression or thoughts of self-harm,” while also addressing “transportation problems, food insecurity, grief” and other behavioral health needs. City leaders explained that the center “relieves the burden on EMS, on the emergency rooms, on police… who otherwise were the first resort for these [calls for service],” creating a new option for people in crisis.

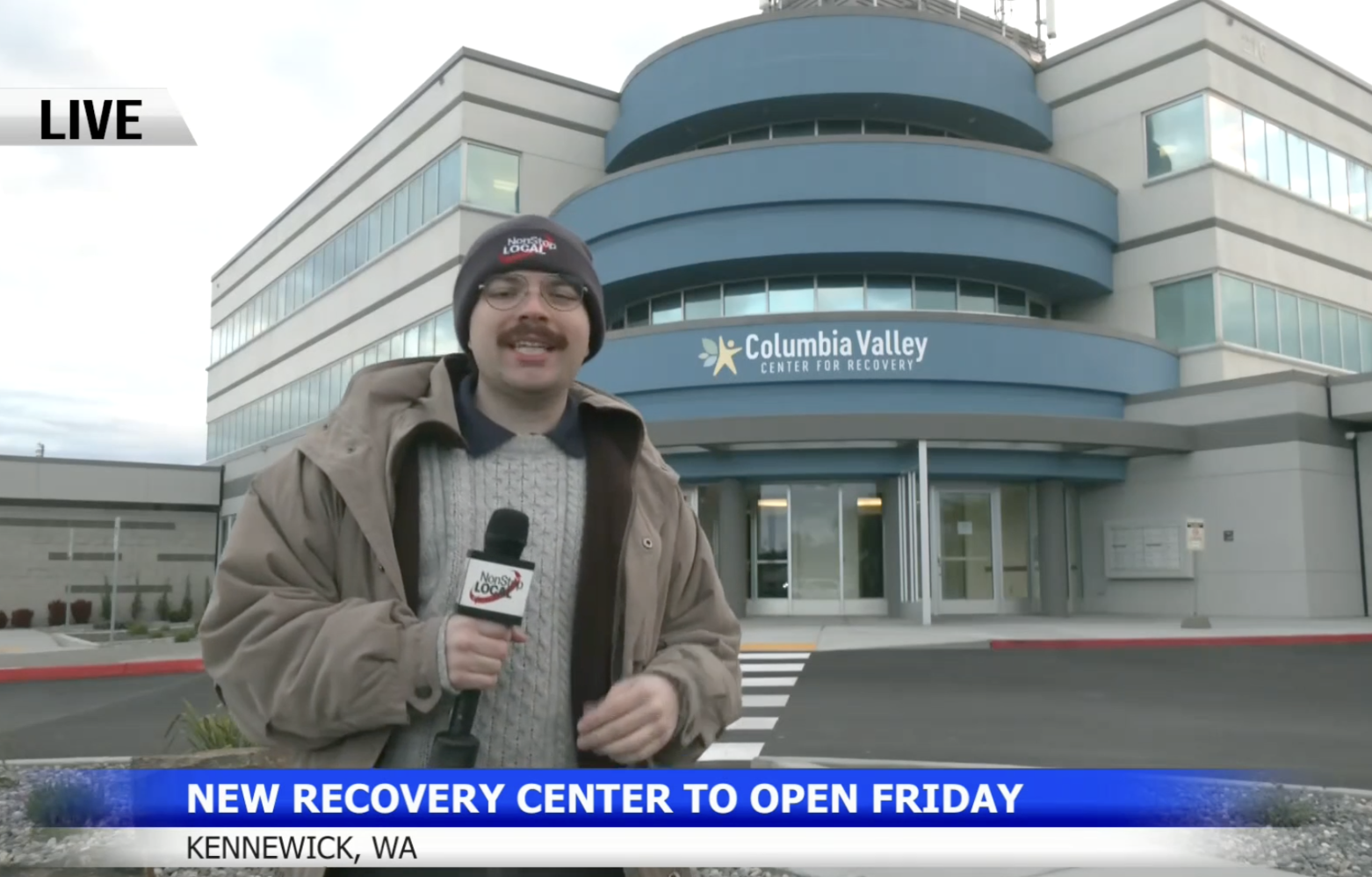
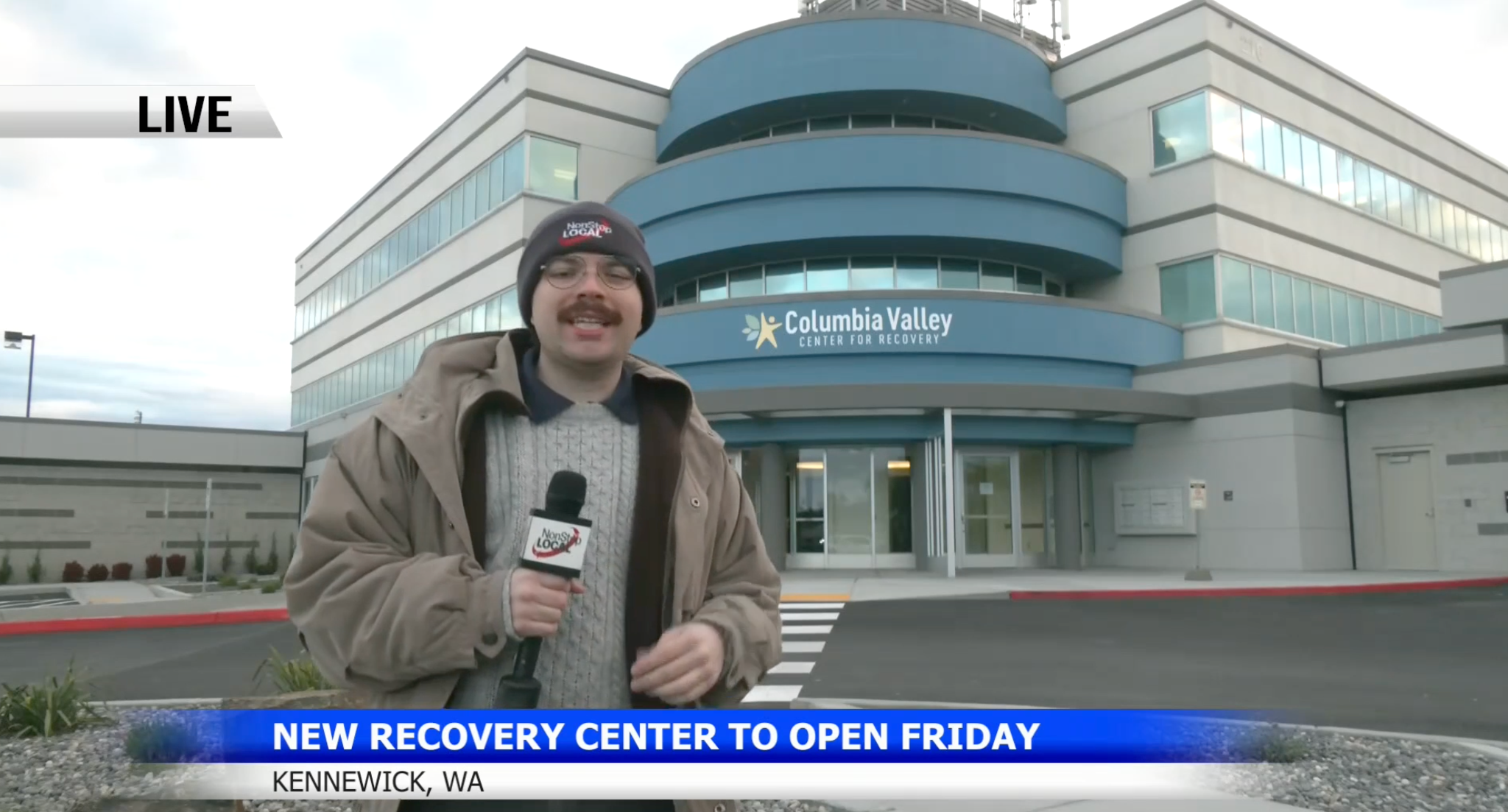
- In Kennewick, Washington, New Center To Offer “Another Option Beyond A Jail Cell Or The Emergency Room.” For NBC News, Christopher Wright reports on Kennewick’s opening of the Columbia Valley Center for Recovery with a “no-wrong-door, 24/7 approach” for people facing addiction and behavioral health crises. The first phase includes “a mental health unit, a voluntary unit, an involuntary unit, crisis stabilization, and on-location healthcare staff.” County leaders said the goal is to give residents “another option beyond a jail cell or the emergency room. Michele Gerber, president of the Benton Franklin Recovery Coalition which oversees the facility, explained to the news station that the project was inspired by “personal loss and years of watching [her son] struggle… ‘my son developed addiction as a teenager and he was in addiction for more than 20 years… [so] the philosophy here is that addiction is a disease. It’s not a disgrace. It’s not a moral issue. It’s a medical issue… People have to be given a chance to have hope and a new beginning, not just punishment.’”
- San Diego County Opens First East County Crisis Stabilization Unit As A “More Effective Option” Than Hospitals And Jails. For San Diego County News Center, Anita Lightfoot reports that San Diego County is opening its newest Crisis Stabilization Unit in El Cajon—the first located in East County. The new 14,000-square-foot facility offers “24/7 support and treatment for people experiencing a psychiatric or substance use emergency,” providing “a calm, safe environment” where residents can receive immediate care and connect with ongoing services. As Lightfoot notes, this center is part of an ongoing effort to establish more crisis stabilization centers across the county with this new $28 million center in El Cajon being the eighth CSU county leaders have launched, with the goal of offering “a more effective option for urgent behavioral health care than emergency departments, hospitals or jails.”