1. Portland Street Response Team Marks Major Milestone—Responds To More Than 50,000 Calls For Service. Portland’s lauded mobile crisis response team, which has recently expanded into a community safety-style department that is an “equal part of the city’s public safety system, alongside police and fire” has responded to more than 50,000 calls for service, the city’s team tracker reported. Here’s a look at the city’s data below (you can visit their dashboard and dive deeper here):
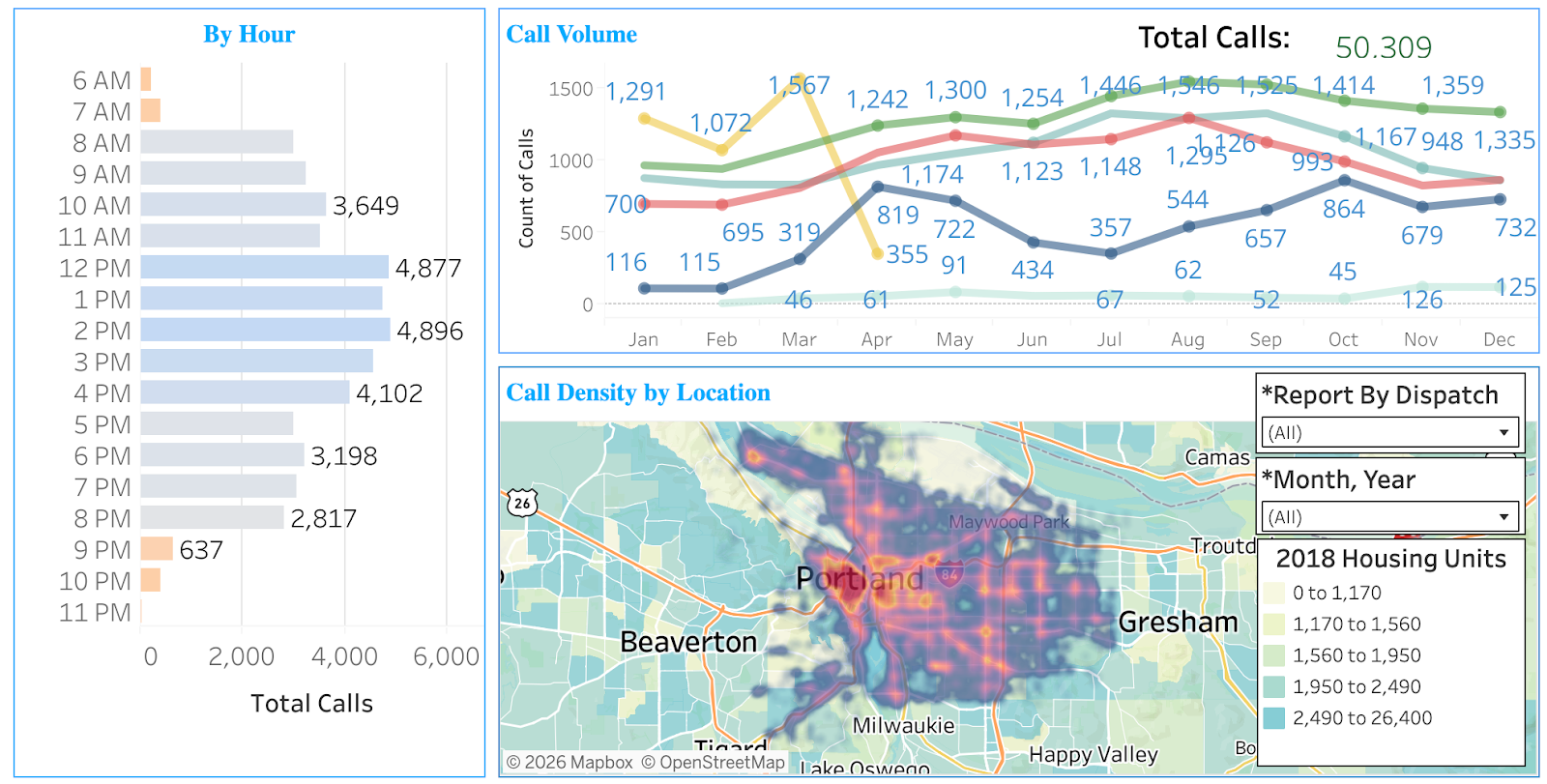
For KATU, Victor Park reports that the team is part of a “national shift” in how cities are responding to mental health and behavioral health emergencies, responding to “thousands of low-risk 911 calls [instead of] police.” And the demand for the team is growing—in 2022, the team “responded to just over 6,000 calls,” KATU noted, but that has grown each year. “Last year, that number skyrocketed” to more than 15,000. Since the team launched in 2021, it has responded to more than 50,000 calls and “only 82 required a police response and around 750 patients required a visit to the emergency room, meaning most crises are resolved on scene,” KATU reported.
Portland Street Response just celebrated its fifth anniversary last month, with city leaders saying that the program “has grown into an essential pillar of Portland’s public safety system.” The team, composed of highly trained mental health professionals, “brings an emphasis on de-escalation, support, and follow-up… to resolve emergencies that don’t fit neatly into categories that were designed 100 years ago.”
Portland Mayor Keith Wilson, a champion of the team, said that PSR is “a vital part of our public safety system… PSR can help folks in a way that no other service provides…. they’re effective, reliable, and humane… and they free up our police officers and firefighters to respond to other calls.”
Last year, Wilson expanded the team with more “operating hours and added money for more PSR responders… and last summer, City Council adopted a resolution recognizing PSR as an equal branch of Portland’s first response system, authorized to respond to 911 calls independently, or alongside other first responders when appropriate.” Now with a budget of $10 million, the team responds to calls for service seven days a week and can “shuttle folks to resources like shelters, day centers, and drug treatment.” Its staff receives the full “designation as first responders, with all the associated [employment] benefits,” and the team “get direct dispatch through 911.”
The Portland Police Bureau explained to KATU the vital role that PSR plays in the public safety infrastructure of the city:
“PSR is a great public safety partner and we’re sincerely grateful for the work they do. Officers frequently encounter situations that a law enforcement solution, such as a criminal charge, is not the best. They recognize that. Every day I hear on the radio officers requesting PSR response to help with people who need it. In the course of our work, we frequently encounter those who have challenges related to their mental and physical health, addiction, housing, and so on… We know that uniformed police officers are incredibly important, but we are not the best responder for every situation. We’re glad when there is a more effective solution available so we can concentrate on what we do best.”

More Momentum For Mobile Crisis Teams Around The Country:
- In Nashville, Tennessee, Fire Department And Clinicians “Team Up For 24/7 Mental Health Calls. . . In Its First 100 Days, It’s Changed Lives… Freed Up Emergency Resources.” For News Channel 5, Aaron Cantrell reports that in its first 100 days, the REACH team—a 24/7 mobile crisis response team that “pairs mental health counselors with fire and EMS crews to assist people in crisis”—has already “changed lives, diverted ER visits and freed up emergency resources.” In the first 100 days in operation, “two-thirds of calls were diverted… into mental health treatment” allowing for emergency responder resources to be freed up for use in other emergencies instead. Prior to the REACH team launch, “there was no immediate resource for mental health calls,” but now, mental health experts respond and “can design crisis plans that connect people with outpatient care, help them stay at home or link them with a [crisis] stabilization unit.”
- Ann Arbor, Michigan, Advances SPROUT Crisis Response Team That Sends Mental Health Experts, Instead Of Police, To Some 911 Calls. The Michigan Daily reports on the City Council moving forward with the launch of a new mobile crisis response team that sends mental health experts “to respond to emergency calls relating to non-violent mental health crises… instead of sending police officers.” To get a jump on development of the program, the city is considering a partnership with Washtenaw County Community Mental Health program, an existing mental health care service that provides “behavioral health services for [] residents with intellectual or developmental disabilities, mental health concerns and substance use issues… [and] operates a 24/7 crisis hotline, and in 2024, they responded to 6,306 mental health crisis calls.”
- In Whatcom County, Washington, Youth-Focused Mobile Crisis Response Team Expands. For The Bellingham Herald, Hannah Edelman reports that the YGo mobile crisis team will expand its operations in the county and to nearby Skagit and Snohomish counties “seven days a week rather than just weekdays.” The team, “helps individuals under 20 and their families, providing services outside of school hours… [and] also work with kids who are struggling in school, being discharged from the hospital following a crisis, involved in the justice system or dealing with child protective services,” with the goal of “keeping them in their current environment rather than having them go to the emergency room or law enforcement, which don’t often address long-term needs or deal with the family unit as a whole.” What makes the team unique compared to other emergency responders in the region is they can “work with families for up to eight weeks … [and] often involve youth peers for support and, uniquely to the program, parent peers [who] bring their own lived experience of raising kids with behavioral health issues and navigating the system.”
2. Crisis Stabilization Centers Expanding Across The Country, As Cities Build 24/7 Alternatives To ERs And Jails.
- In Newark, New Jersey, State’s First Crisis Stabilization Center Set To Open “For People In Mental Health, Drug Crisis.” For The New Jersey Monitor, Lilo Stainton reports on New Jersey’s first crisis stabilization center, a partnership between the state and Rutgers University, where people experiencing a mental health or substance use crisis “can get medication, professional and peer support, and a comfortable place to rest for up to 24 hours.” The center is a “final link” in the modernization of both Newark’s and New Jersey’s public safety infrastructure that Governor Mikie Sherrill and Newark Mayor Ras Baraka have been instrumental in the effort to build, as Safer Cities has previously covered. The center—which will “save taxpayer money by reducing the burden on more costly options, like emergency rooms and correctional facilities”—will “be open 24 hours every day, is designed to be a less stressful alternative to a hospital emergency room and features private clinical rooms and comfortable lounge chairs… is open to all, regardless of anyone’s ability to pay.” The center adds to a comprehensive suite of expanded public safety services including an Office of Violence Prevention that takes a public health lens to gun violence reduction, a longstanding community-based and hospital-based violence intervention; homelessness outreach; and mental health mobile crisis responder team.
Stephen Cha, the commissioner of the state’s Department of Human Services, explained the importance of the center as a core component of the state’s services: “People need somewhere to call. People need someone to respond, but also people need somewhere to go, and that’s what this place is here.” This is the first of five centers opening in the state, with four more planned for Morris, Bergen, Monmouth, and Camden counties.


- Madera County, California, “Breaks Ground On New Crisis Stabilization And Sobering Center… An Alternative To Jail, Overcrowded Emergency Rooms.” For Fox 26 News, Dania Romero reports on the new $27 million facility that is “designed to provide immediate care for individuals experiencing mental health or substance use emergencies… an alternative to [being taken to a] jail or overcrowded emergency rooms… to reduce strain on first responders, and provide more appropriate treatment options for people in crisis.” The facility, which is expected to open next year, will include “dedicated mental health treatment rooms and … beds for individuals receiving care for substance use disorders… [and] also help tackle related issues such as homelessness.”

- Spokane County, Washington Breaks Ground On New Crisis Stabilization Center,
“Considered ‘Beacon Of Hope’ In Combating Addiction, Mental Health Crises.” For The Spokesman Review, Nick Gibson reports on the $21 million, 17,000 square foot facility that will provide a suite of treatment “services for mental health and drug addiction” including “crisis relief, sobering, stabilization, withdrawal management and co-occurring treatment,” while also reducing strain on jails and hospitals. The new facility, expected to open next year, will be a significant expansion of available mental health and addiction treatment beds in the region, which local leaders explained to the paper remain at maximum capacity. Justin Johnson, director of the county’s community services department, explained the important function this facility will play for increasing public safety and improve treatment outcomes: “When an individual is in crisis, they often get lost in a complex system… either in the criminal, legal system, or they find themselves in an overburdened ER. What we’re trying to do here is address that [ensuring people] receive care, when they need it, in one location.”
3. Study: Business Leaders, Service Providers Say That Health Experts, Rather Than Police, Are Better Positioned For Effective Overdose Response. A new study published in the Journal of Community Health by researchers from New York University School of Global Public Health and Brown University surveyed 100 business employees and service providers in Rhode Island overdose hotspots to understand attitudes toward police involvement in overdose response. The researchers found respondents highly valued police for general safety, but were far less likely to view them as effective for overdose response functions. The full study is worth your time, but here are the toplines:
- Police Presence May Deter Life-Saving Help: The study notes that “police presence at overdose scenes can deter life-saving help-seeking behaviors due to fear of legal consequences,” and that when police arrive, life-saving interventions occur “in the context of potential arrest and incarceration of overdose survivors and their networks.” Researchers say this creates “a core discrepancy” between public health–focused overdose response and traditional enforcement approaches, helping explain why respondents viewed health-focused responders as better suited for these incidents.
- Opportunity For Specialized Response Teams To Improve Effectiveness: The researchers found that “there may be appetite to modify the role of police to focus more on public safety in overdose response or social services linkages,” and that “substantially lower share of individuals who believe police presence potentiates overdose prevention and service linkage demonstrates there is a receptive audience for testing alternatives.” The authors emphasize that clinicians, outreach workers, and harm-reduction professionals are best suited to lead overdose response to improve outcomes.
- Businesses In Overdose Hotspots Are Providing Narcan Training To Staff. Researchers report “48% reported that some or all staff at their workplace had received [Narcan] training,” while “35% indicated their organization had measures or protocols in place for overdose prevention and response.” Additionally, “37% reported that an overdose had occurred at their workplace location at some point,” underscoring the frequency of these incidents and highlighting the strong need for dedicated, specialized response teams equipped to handle overdose emergencies quickly and effectively.
Spotlight On Cities With Overdose Responder Teams:
- In Caldwell County, North Carolina, PORT Overdose Response Team Combines “Paramedics And Certified Peer Support Specialists” To Respond To 911 Overdose Calls. As the county describes, the “paramedic renders clinical care, if needed, and the peer support specialist offers support and guidance to the individual.” The team then follows-up with anyone who has experienced an overdose within 72 hours of the incident to make sure they are stable and provide additional treatment or connection to services.
- In Milwaukee, Wisconsin, Overdose Response Team Part Of Effort That “Reduced Overdose Deaths To Their Lowest Numbers In A Decade.” For News From The States, Isiah Holmes reports on the city’s overdose response team, which launched in 2019, and has become a core piece of the city’s public safety infrastructure, providing better outcomes for people experiencing overdoses, and reducing strain on law enforcement and other first responders. Housed in the Fire Department, and composed of fire department medics and addiction peer support specialists who respond to 911 calls for service around overdoses, the team will respond to acute overdoses and then follow up with people who “had survived an overdose within the last 24-48 hours.” From there, the overdose team “regularly works to get people into treatment programs… [as well as] getting someone clothes, food, providing them with narcan” and other support and connection to services.

In Albuquerque, New Mexico, Community Safety Department And Fire Department Collaborate On Overdose Response Team. The program pairs firefighters and behavioral health responders to deliver “medication for Opioid Use Disorder… as quickly as possible, followed by transport to local treatment facilities,” helping “reduce the risk of repeat overdoses and support long-term recovery,” the city announced. In a recent response, firefighters administered Narcan and buprenorphine on scene, while behavioral health responders provided follow-up support and transportation to treatment. The team “helps stabilize patients in crisis, reduces unnecessary emergency department transports, and improves connections to follow-up care, benefiting both individuals and the broader healthcare system.”
